Cumulative Benefits
of HBOT
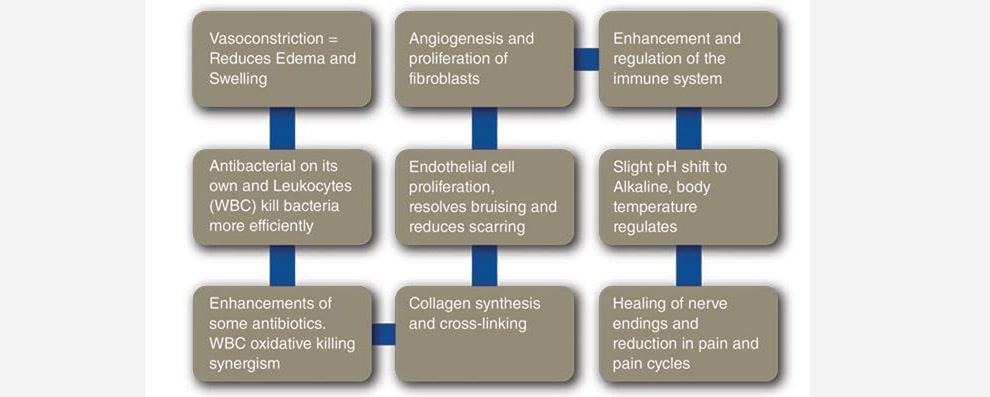
Decades of research and US Wound Registry data demonstrate that following a prescribed HBOT protocol has these cumulative physiological benefits.
Principal Mechanism
“Principal mechanisms of HBO2 are based on intracellular generation of reactive species of oxygen and nitrogen. Reactive species are recognized to play a central role in cell signal transduction cascades…” Source Article
“Most controlled studies have verified that the clinical efficacy from HBO2 derives from modulation of intracellular transduction cascades, leading to synthesis of growth factors and promoting wound healing and ameliorating post-ischemic and post-inflammatory injuries.”
Source Article
Neurological Mechanism
“Known mechanisms of HBOT-induced neuroprotection include enhancing neuronal viability via increased tissue oxygen delivery to the area of diminished blood flow, reducing brain edema, and improving metabolism after ischemia [28,29]. Furthermore, a recent study performed on a rat suggested that upregulation of the expression of glial derived neurotrophic factor (GDNF) and nerve growth factor (NGF) might underlie the effect of HBOT [30].”
Source Article